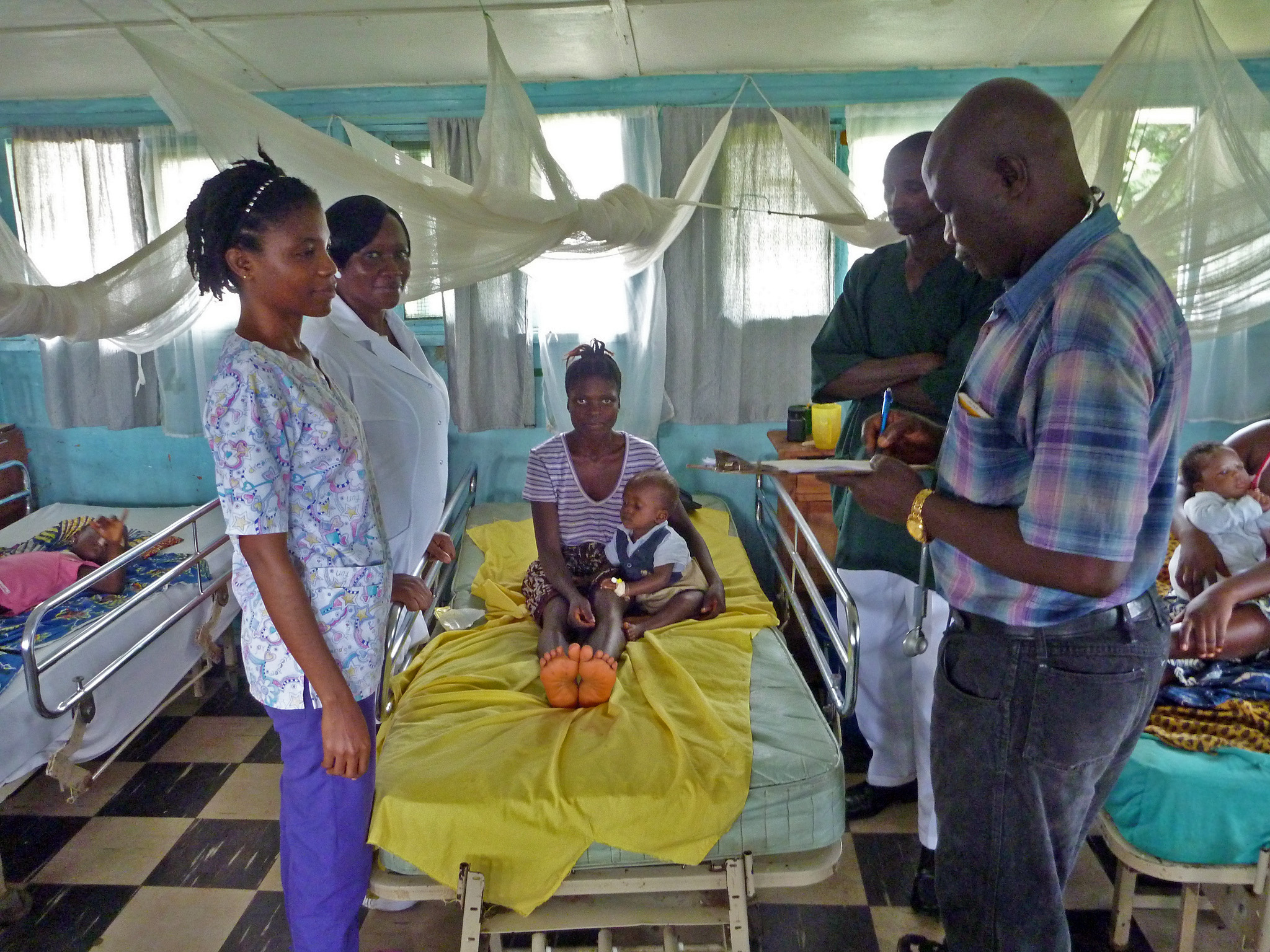
Liberia, West Africa
BACKGROUND
Founded in 1847, Liberia is the oldest republic in Africa. Liberia has come a long way in since the end of its civil war. In 2003, the country lay in ruins after 14 years of conflict. Few Liberians were untouched by the violence. Out of a population of 3.5 million, an estimated 270,000 people lost their lives, and more than 800,000 were displaced. Young people were traumatized by the war, in which many children enlisted as soldiers in the various rebel groups that marauded their way up and down the country. Liberia’s infrastructure was shattered, with roads and bridges destroyed and water and power supplies cut. The health and educational systems were not spared. Hospitals, clinics, and schools were looted and burned down or vandalized. By the end of the war:
only 354 health facilities remained operational, out of a prewar total of 5505.
Nine out of ten doctors had fled the country, and the medical training system had collapsed.
Just 168 physicians remained, mostly in Monrovia, for a population of over 3.5 million people
The war had a catastrophic impact on Liberia’s health, education, and development indicators. Per the 2007 Demographic and Health Survey:
infant mortality rate of 71 deaths per 1,000 live births
Only 39 percent of children under the age of two had received their recommended vaccinations
One in every nine children died before his or her fifth birthday.
maternal mortality rate was 994 deaths per 100,000 live births
Liberia continues to be one of the world’s poorest countries, ranked 162nd out of 169 countries in the 2010 United National Development Program Human Development Index, And After the Ebola Crisis ranked No. 1 by USA TODAY in 2018. between 64% and 84% of the population live in extreme poverty, defined as less than $1.25 day.
A National Health Policy (NHP), published in 2007, was integrated with the government’s Poverty Reduction Strategy, a blueprint for adding impetus to Liberia’s postwar recovery from 2008 to 2011. The center- piece of the NHP was a plan to deliver a basic package of health services (BPHS), free of charge, to Liberian citizens. These services included communicable disease control, emergency care, maternal and newborn health, and mental health care.
Fast forward to 2014, and signs of progress are everywhere. The resumption of basic health services has begun to have a positive impact on health outcomes. Sixty-four percent of children under the age of two have been immunized compared with 35 percent in 2003.
Liberia has seen improvements in the under-five mortality (U5M) rate, which declined from 220 deaths per 1,000 live births in 1986 to 110 deaths per 1,000 live births in 2007; however, this U5M rate of 110 is still high. Child health in Liberia still faces daunting challenges, most notably chronic undernutrition, as the stunting prevalence has steadily risen over the last decade and is currently measured at 42 percent.
The MoHSW broadened its scope, launching an essential package of health services (EPHS) in 2011. The EPHS widens the number of services the government commits to providing to include treatment for noncommunicable diseases, child nutrition, dental and eye care, and neglected tropical diseases. The EPHS also aims to strengthen the referral system, formalizing a tiered structure of primary, secondary, and tertiary facilities with the objective of rationalizing services and making the system more efficient.